By Dr. Belinda Gregory-Head, DDS, Dental Implant Partners, San Francisco
As a prosthodontist practicing in San Francisco for over 15 years, I’ve worked with thousands of patients considering restorative options for missing teeth. Among the most commonly compared treatments are dental implants and dentures. While both can restore oral function and appearance, the differences in biomechanics, materials, long-term outcomes, and patient satisfaction are substantial. This guide is written from a clinician’s point of view to help patients and professionals alike understand the nuanced clinical factors involved in making the best decision.

Understanding the Fundamentals: What Are Dental Implants and Dentures?
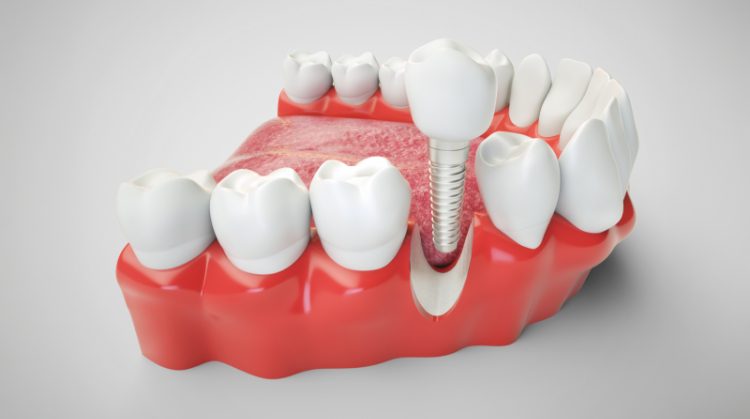
Dental implants are titanium or zirconia posts surgically inserted into the jawbone, functioning as artificial tooth roots. They osseointegrate, meaning they biologically bond with the surrounding bone tissue, providing a stable base for prosthetic teeth. This treatment is typically chosen for single-tooth replacement, bridges, or full-arch reconstructions supported by multiple implants. Implants mimic the mechanical load of natural teeth and help maintain the health of the jawbone by preventing bone resorption.
Dentures, by contrast, are removable prosthetic devices made from acrylic, resin, and sometimes metal, designed to replace missing teeth and surrounding tissues. Full dentures replace all teeth in an arch, while partial dentures fill gaps between remaining natural teeth. They rest on the gums and are supported either by suction, clasps, or adhesives. Because they are not anchored into bone, their retention and function rely more on soft tissue adaptation and mechanical design.
From a prosthodontic standpoint, these two modalities differ significantly in how they interact with oral anatomy. Implants restore lost biomechanical function by transferring occlusal forces directly to the alveolar bone. Dentures distribute these forces across the mucosa, which was never biomechanically intended to handle such stress, often leading to tissue irritation and bone atrophy over time.
Bone Preservation and Jaw Health
One of the most critical advantages of dental implants is their ability to preserve the alveolar bone. The absence of natural teeth leads to disuse atrophy of the jawbone, a phenomenon known as alveolar ridge resorption. This is particularly rapid within the first year post-extraction and continues over time. Implants halt or even reverse this bone loss due to the functional loading they provide, which stimulates bone remodeling through Wolff’s Law.
Conversely, dentures accelerate the rate of bone resorption. Without mechanical stimulation, the body begins to resorb the bone underlying the denture. In the maxilla, this can lead to sinus pneumatization and loss of vertical facial dimension; in the mandible, progressive resorption can compromise denture stability and patient comfort. These changes not only affect prosthesis fit but also facial esthetics and phonetics.
In patients who have been edentulous for several years, the resulting bone loss can become so advanced that surgical bone grafting may be required prior to implant placement. As a prosthodontist, I often stress the importance of timely implant placement to mitigate these long-term degenerative changes and reduce the need for extensive future interventions.
Functional Efficiency and Chewing Capability
Implants far exceed dentures in terms of masticatory efficiency. Studies consistently show that implant-supported prostheses restore up to 90% of the natural bite force, while conventional dentures restore only about 20–30%. This disparity directly impacts a patient’s ability to chew fibrous foods like meats, raw vegetables, and nuts an important consideration for nutritional health.
Denture wearers often adapt by shifting their diets to softer, more processed foods. This can lead to imbalanced nutrition, especially in elderly populations who already face dietary challenges. Implant-supported prostheses, whether single crowns, bridges, or full-arch hybrids, allow patients to enjoy a varied diet with confidence and minimal restriction.
Additionally, implant stability prevents movement during function. Even well-designed dentures may shift or rock under occlusal load, causing discomfort and embarrassment. In contrast, implants anchor the prosthesis firmly to bone, preserving occlusal harmony and reducing the neuromuscular adaptations required to use removable appliances.
Esthetics and Facial Support
Dental implants allow for highly customized, natural-looking restorations. Each crown or prosthesis can be individually designed to match the shape, color, translucency, and alignment of natural dentition. Because they emerge directly from the gingiva, implant restorations often have a lifelike appearance that mimics natural teeth in emergence profile and contour.
Dentures, especially conventional ones, often fall short in this regard. They can appear bulky, especially in the anterior region, and may shift during speech or laughter. Over time, as bone resorption progresses, the facial support provided by dentures diminishes. This can result in a sunken, aged appearance due to loss of vertical dimension and soft tissue collapse.
From an esthetic and prosthodontic standpoint, implants provide superior facial support by maintaining the vertical dimension of occlusion and restoring midface fullness. Full-arch implant solutions such as All-on-4 or bar-retained overdentures also allow for lip support customization without the instability issues of conventional dentures.

Comfort and Oral Sensation
Comfort is a significant factor for patient satisfaction. Implants integrate with bone and have no contact with soft tissues during function, which often makes them feel like natural teeth. They do not trigger gag reflexes, impede tongue space, or cause sore spots. After healing and prosthetic integration, most patients report forgetting they even have implants.
Dentures, in contrast, sit on the mucosa and are retained by suction or adhesives. This contact often leads to sore spots, ulcers, and discomfort particularly in patients with thin or atrophic ridges. Poorly fitting dentures can create chronic irritation and lead to mucosal hyperplasia or candidiasis. Even well-fitting dentures need periodic relining as tissue changes occur.
Moreover, implants allow for improved proprioception, the sensory feedback that guides bite force and jaw positioning. While they don’t fully restore the periodontal ligament function, osseointegrated implants transmit mechanical signals through the bone, which is far superior to the sensory void created by removable appliances.
Maintenance, Hygiene, and Long-Term Care
Implant restorations require diligent oral hygiene but are relatively low-maintenance compared to removable prosthetics. Patients must maintain regular brushing, flossing (or use of interdental brushes/water flossers), and periodic professional cleanings to prevent peri-implantitis, a condition akin to periodontal disease in natural teeth. However, with good maintenance, implant longevity is outstanding, with 10-year survival rates exceeding 95%.
Dentures demand daily removal, soaking, and meticulous cleaning. Failure to do so can result in fungal infections, halitosis, and biofilm accumulation. Additionally, dentures must be periodically relined or remade every 5–7 years due to ongoing bone resorption and wear. The long-term upkeep of dentures can become both labor-intensive and costly.
As a clinician, I emphasize that while implants may require a greater upfront commitment, their maintenance tends to be more predictable and hygienically manageable for most patients. It’s essential to tailor hygiene protocols to the patient’s dexterity, medical status, and prosthesis type for long-term success.
Surgical Considerations and Healing Time
The surgical aspect of implant therapy often deters some patients initially, but when properly planned, the procedure is minimally invasive and highly successful. Implant placement typically involves a single-stage or two-stage surgery under local anesthesia, with optional sedation. Modern digital planning using CBCT imaging and surgical guides has made the process highly precise.
Healing times can vary. Traditional implant protocols may require 3–6 months of osseointegration before loading, though immediate-load protocols are available for certain cases. Patients with systemic conditions, such as uncontrolled diabetes or smoking habits, may require longer healing and more conservative approaches to ensure implant success.
Dentures, by contrast, are non-surgical and can be fabricated relatively quickly, sometimes even as immediate dentures on the day of extractions. However, the convenience is offset by their frequent need for adjustment as the bone remodels. Patients often mistake speed for efficacy, but long-term outcomes should take precedence over short-term expediency.
Financial Investment and Cost-Effectiveness
Implants represent a higher initial cost investment, especially when bone grafting or full-arch reconstruction is involved. However, the long-term value is generally superior due to their longevity and minimal need for replacement. When amortized over a 20+ year period, implants are often more cost-effective than repeatedly replacing or adjusting dentures.
Dentures are less expensive initially, making them appealing to patients on a tighter budget. However, frequent relining, repairs, replacements, and the cost of adhesives or comfort products can accumulate. Additionally, the impact on quality of life ranging from diet limitations to social discomfort should be considered part of the real “cost.”
Many practices, including ours at Dental Implant Partners, offer phased treatment planning and financing options to make implant care more accessible. It’s also important to factor in insurance limitations and medical necessity documentation when considering reimbursement or Health Savings Account coverage.
Psychological and Quality-of-Life Outcomes
From a psychological perspective, implants tend to offer significantly greater satisfaction and confidence. They allow patients to speak, chew, and smile without fear of movement or embarrassment. Studies show a marked improvement in self-esteem and social participation in patients who transition from dentures to fixed implant restorations.
Denture users often report self-consciousness, especially in social or professional settings. This is compounded by functional issues such as clicking sounds, slippage, or even accidental dislodgement. These incidents, while common, have a profound effect on mental well-being and quality of life.
Prosthodontics is not just about restoring anatomy it’s about restoring identity. As a clinician, I’ve witnessed the profound transformation patients experience when transitioning to implant-supported restorations. Confidence, social engagement, and even professional performance often improve dramatically following treatment.
Patient Candidacy and Clinical Decision-Making
Not every patient is a candidate for implants, and clinical judgment is essential. Factors such as bone volume, systemic health, smoking status, and financial capacity must be carefully evaluated. Pre-implant assessments often include CBCT imaging, periodontal evaluation, and sometimes laboratory blood panels to assess healing potential.
For patients with complex medical histories or severe bone loss, dentures may remain the more practical option. However, in many cases, a hybrid approach, such as implant-retained overdentures, can offer a middle ground by improving retention while minimizing cost and surgical burden.
As prosthodontists, we have a duty to tailor treatment to each individual’s anatomical, functional, and psychosocial needs. It is not a binary choice, but a nuanced decision made through comprehensive diagnosis, patient education, and shared goals. At Dental Implant Partners, we use a multidisciplinary approach that ensures each patient receives a customized, evidence-based solution.
Final Thoughts: Empowering Informed Choices
The decision between dental implants and dentures is deeply personal, but it should be guided by clinical insight, long-term planning, and individualized care. While implants offer superior outcomes in nearly every domain function, esthetics, longevity, and comfort dentures still have a place in the prosthodontic arsenal for select patients.
My advice, as always, is to consult with a specialist who can evaluate your unique situation using advanced diagnostics and comprehensive treatment planning. If you’re in the San Francisco area, I welcome you to visit us at Dental Implant Partners for a full consultation. Empowering patients with knowledge is the first step toward a restored smile and a renewed sense of self.

About Dental Implant Partners
At Dental Implant Partners, this work is not just our profession; it’s our passion. For over 25 years, I’ve had the privilege of leading a dedicated prosthodontic practice rooted in the heart of San Francisco. What began as a solo practice has grown into a collaborative team of highly trained prosthodontists, general dentists, and dental hygienists who share a deep commitment to patient-centered, comprehensive care. Each member of our team brings years of focused experience in restorative dentistry, allowing us to provide personalized solutions ranging from simple fillings and veneers to full-mouth reconstructions supported by dental implants.
Our approach to care is both thoughtful and thorough. Whether you’re considering dental implants to restore function or need expertly crafted dentures tailored to your anatomy and lifestyle, our clinical decisions are grounded in evidence, experience, and genuine care. For patients who are not candidates for implants, we offer expertly designed removable prostheses that prioritize function and esthetics without compromise. Our dental hygienists, many of whom trained as dentists, are known for their precision, warmth, and the long-term relationships they maintain with our patients. This continuity of care ensures that your oral health remains in expert hands, no matter the complexity of your needs.
If you’re exploring your options between dental implants and dentures, I invite you to schedule a consultation with us at our beautiful San Francisco office overlooking the Bay. We would love to help you find the right treatment path, restore your smile, and support your oral health for years to come. Reach out today to take the next step toward a confident, functional, and healthy smile.