By Dr. Belinda Gregory-Head, DDS – Dental Implant Partners, San Francisco
As a prosthodontist and restorative dentist, I often work with patients who have experienced significant deterioration of their oral health, whether due to trauma, decay, systemic illness, or congenital conditions. Full mouth reconstruction (FMR) is a comprehensive, multidisciplinary treatment approach that aims to restore both function and aesthetics to the entire dentition. It is not simply a cosmetic enhancement; it becomes essential when a patient’s ability to chew, speak, or maintain healthy occlusion is compromised.
FMR requires an advanced understanding of the relationships between occlusion (bite), temporomandibular joint (TMJ) function, periodontal health, and the structural integrity of the teeth and supporting bone. Each treatment plan is tailored to the individual and may involve specialists in prosthodontics, periodontics, endodontics, orthodontics, and oral surgery. As a dentist with extensive training in restorative and implant dentistry, I approach every case using current evidence and best practices, focusing on long-term functional and aesthetic outcomes.
FMR is a long-term journey that often spans several months or even years. Accurate sequencing, diagnostic precision, and strong patient engagement are essential throughout the process. My role is to guide patients through each phase of treatment, ensuring that every step is purposefully aligned with the next, and that patients are fully informed about what to expect from beginning to end.

Dental Crowns: Rebuilding Strength and Structure
Dental crowns are essential in FMR, especially when addressing severely worn, fractured, or previously root canal-treated teeth. A crown provides full coverage of the tooth, restoring its original size, shape, strength, and appearance. Material selection is critical and based on multiple factors such as location, functional load, and esthetic demands. In molar regions, I often choose monolithic zirconia due to its durability, while anterior crowns may be fabricated from layered ceramics for superior translucency and lifelike appearance.
At my San Francisco clinic, we always begin with diagnostic wax-ups and digital scans to ensure precision and accuracy. Crowns must be integrated into the patient’s overall bite scheme, which requires careful analysis of the vertical dimension of occlusion, functional range of motion, and occlusal balance. When restoring an entire arch or full dentition with crowns, I evaluate whether to incorporate canine guidance or group function, particularly for patients with bruxism or other parafunctional habits that increase stress on restorations.
Preserving natural tooth structure remains a priority. Modern adhesive technologies and conservative prep designs allow us to create durable crowns while retaining enamel where possible. A well-designed crown, placed with proper occlusal considerations and supported by healthy periodontal tissues, can restore function and esthetics while significantly extending the longevity of the tooth.
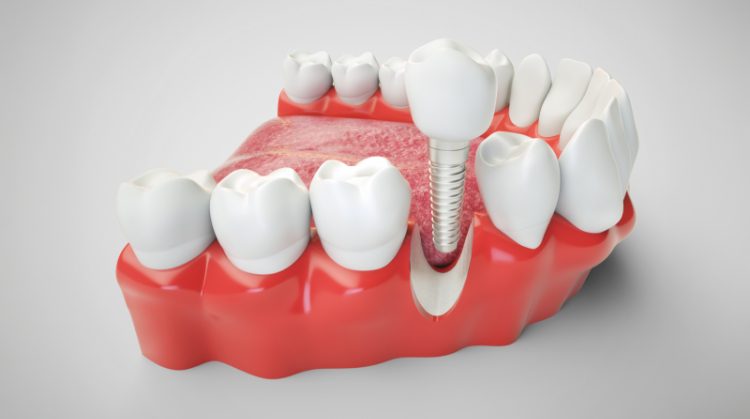
Dental Implants: The Gold Standard for Missing Teeth
Dental implants represent the most stable and biologically integrated solution for replacing missing teeth in FMR. Unlike bridges or dentures, implants replace the entire tooth structure including the root, which maintains bone health, supports facial structure, and improves biomechanical loading. In my practice, implants are transformative for patients who have lost function and confidence due to missing or failing teeth.
Successful implant planning begins with detailed diagnostics, including cone beam CT imaging, intraoral scans, and digital planning software. In full arch scenarios such as All-on-4, All-on-6, or hybrid prostheses, proper implant distribution is critical to avoid overload and ensure even stress distribution across the arch. Patients with bone loss may also require preparatory procedures such as sinus augmentation or guided bone regeneration to support optimal implant positioning.
Implant restorations vary widely depending on the clinical presentation. Options include single-tooth implants, implant-supported bridges, and screw-retained full arch prostheses made of zirconia or acrylic materials. I frequently collaborate with digital labs to pre-plan the definitive prosthesis and sometimes fabricate immediate load temporaries for select cases. This level of planning enhances surgical efficiency and ensures prosthetic precision, improving both short-term comfort and long-term results.
Veneers: Aesthetic Correction in a Functional Framework
Veneers are often viewed as cosmetic solutions, but they serve an important role in FMR for patients with structurally sound anterior teeth that require aesthetic and functional improvement. For teeth affected by intrinsic discoloration, incisal wear, or slight misalignment, veneers can restore appropriate form and guidance without removing excessive enamel.
Before recommending veneers as part of FMR, I evaluate their contribution to anterior guidance. This guidance is critical for protecting posterior restorations by facilitating proper disclusion during excursive movements. I employ digital smile design and chairside mock-ups to preview the outcome and make functional adjustments before finalizing the preparation. Proper evaluation ensures that veneers not only look natural but also contribute to a stable occlusal scheme.
Material selection is equally important. I often prefer lithium disilicate for its strength and translucency, although feldspathic porcelain may be used in cases where ultra-thin preparation is preferred. Bonding protocols are strictly adhered to, and occlusal forces are carefully evaluated. When well-integrated into the broader FMR plan, veneers can deliver predictable, long-lasting esthetic and functional results.
Bridges and Fixed Partial Dentures: Strategic Tooth Replacement
While dental implants are the preferred solution for missing teeth, fixed bridges still serve a valuable purpose in FMR for certain patients. Bridges are particularly appropriate when adjacent teeth already require full coverage and when implant placement is contraindicated due to anatomical limitations or medical concerns. When executed with proper planning, bridges can be strong, aesthetic, and long-lasting.
Bridge biomechanics are complex. The span length, location, occlusal forces, and periodontal status of abutment teeth must all be assessed thoroughly. In my practice, I typically limit bridge spans to three units unless the prosthesis is implant-supported. To support longer spans, I often use milled zirconia or reinforced frameworks, and I take care to distribute forces evenly across the arch to reduce stress and prolong the life of the restoration.
There are also more advanced prosthetic options for select cases, such as telescopic bridges or precision attachment dentures, which allow for removable components with improved retention. These designs are appropriate for patients with multiple missing teeth who are not candidates for full-arch implants. Such restorations require meticulous design and fabrication, as well as a high level of hygiene maintenance by the patient.

Orthodontics in Full Mouth Rehabilitation
Orthodontic treatment is often an integral phase of FMR, especially for patients with misaligned, rotated, or extruded teeth that would otherwise compromise restorative outcomes. By aligning the teeth into proper position, we can ensure better load distribution, improved esthetics, and more conservative tooth preparation for crowns or veneers.
I frequently collaborate with orthodontic specialists to coordinate tooth movement that supports the goals of reconstruction. Movements may include intrusion of overerupted teeth, correction of anterior open bites, or de-rotation of malpositioned incisors. These adjustments create a better foundation for final restorations and allow us to work within a more stable functional and esthetic environment.
For adult patients, I often recommend segmental fixed appliances or clear aligners for targeted movements. Orthodontics in this context is not used for cosmetic alignment alone. Instead, every movement is evaluated for its contribution to long-term occlusal balance and restorative success. When incorporated into the FMR sequence, orthodontic treatment can significantly enhance final outcomes.
Periodontal and Soft Tissue Considerations
Healthy periodontal tissues are essential for successful outcomes in FMR. Before initiating any restorative procedures, I conduct a comprehensive periodontal evaluation, including probing depths, clinical attachment levels, and full-mouth radiographs. Inflammation, bone loss, or recession must be addressed prior to placing any long-term restorations.
In patients with excessive gingival display or asymmetrical gum lines, I may recommend gingivoplasty or esthetic crown lengthening to establish ideal gingival architecture. These procedures not only improve esthetics but also provide better emergence profiles for restorations. A balanced soft tissue framework is particularly important for anterior restorations, where tissue symmetry plays a large role in the final appearance.
Keratinized tissue around implants is another important consideration. Lack of attached gingiva may contribute to peri-implant complications and patient discomfort. When necessary, I perform soft tissue grafting to augment deficient areas. These procedures contribute significantly to the longevity of restorations and overall patient satisfaction.
Occlusal Analysis and Bite Reprogramming
Occlusal balance is a cornerstone of FMR. Without proper assessment and correction of bite relationships, restorations are prone to failure from overload, wear, or discomfort. My diagnostic protocol includes mounted study models, facebow transfers, and digital jaw tracking where appropriate. These tools help identify disharmonies in centric relation, vertical dimension, and functional pathways.
Many patients present with a collapsed bite or excessive wear, indicating a need to re-establish the vertical dimension. In these cases, I use deprogramming appliances such as anterior bite planes to help relax the muscles and identify a repeatable and stable jaw position. Once the neuromuscular position is established, we use this as the foundation for building new restorations.
Restorative work must conform to functional parameters. I evaluate incisal guidance, posterior disclusion, and crossover movements to ensure that all prosthetic surfaces are in harmony with the patient’s functional envelope. Ignoring these principles can lead to recurrent fractures or TMJ issues. Careful occlusal planning is essential for comfort, durability, and long-term function.
Digital Dentistry and Diagnostic Technology
The integration of digital tools has revolutionized FMR. In my practice, I rely on technologies such as intraoral scanners, CBCT imaging, digital articulators, and 3D printing to enhance precision and efficiency. These tools allow for better communication between the dental team and laboratory, while also improving patient understanding and treatment acceptance.
Using virtual planning software, we can simulate restorations and implant positions prior to treatment. This level of visualization helps ensure accuracy during surgery and prosthetic fabrication. It also enables us to anticipate complications and adjust the treatment plan before irreversible steps are taken. Digital workflows significantly reduce chair time and improve overall predictability.
For patients, digital previews of their future smile provide motivation and clarity. The ability to show changes in tooth length, alignment, and esthetics in real time fosters better engagement and alignment with treatment goals. By integrating diagnostic technology at every stage, we elevate both the clinical and patient experience.
Maintenance and Long-Term Success
Long-term success of FMR requires ongoing commitment to maintenance and preventive care. After completing treatment, patients must follow a structured hygiene protocol, including professional cleanings, regular bite evaluations, and the use of protective appliances such as night guards where indicated. Restorations may look and feel natural, but they still require diligent care.
Occlusal guards are especially important for patients with a history of bruxism or clenching. These appliances protect restorations from excessive forces during sleep and reduce stress on the TMJs. I fabricate custom night guards for most FMR patients and review wear patterns at follow-up appointments. Adjustments are sometimes necessary to maintain occlusal balance.
Education is a vital part of long-term success. I work closely with patients to teach proper brushing and flossing techniques, discuss dietary choices, and identify habits that could threaten restorative integrity. When patients stay committed to routine maintenance and professional oversight, the results of FMR can last for decades.
Restore Your Smile with Dental Implant Partners in San Francisco
At Dental Implant Partners, full mouth reconstruction is not just a treatment we offer; it is part of the core expertise that defines our practice. For over 25 years, I have had the privilege of leading a dedicated team committed to restorative excellence here in San Francisco. What began as my prosthetic-focused practice has grown into a collaborative group of experienced prosthodontists, general dentists, and hygienists who are deeply invested in providing personalized, high-quality care. Our clinical approach is built on precision, ethics, and long-term thinking, all within a welcoming and state-of-the-art environment that overlooks the San Francisco Bay.
We provide a full spectrum of restorative treatments, from simple fillings to custom veneers to complex rehabilitations involving dental implants. For patients who may not be ideal candidates for implant therapy, we also offer expertly crafted complete and partial dentures. Our hygienists, trained as dentists themselves, bring a unique clinical insight and have been with us for many years, fostering strong and trusted relationships with our patients. Our entire team is aligned in one goal: to restore comfort, function, and confidence through thoughtful and technically excellent dentistry.
If you are considering full mouth reconstruction or simply looking for an experienced team to help guide your dental care, we invite you to connect with us at Dental Implant Partners. We are here to listen, to understand your goals, and to build a treatment plan that is truly tailored to you. We love restoring smiles, and we would love to help you rediscover yours. Reach out today to schedule a consultation.