By Dr. Belinda Gregory-Head, Dental Implant Partners, San Francisco
As a dental professional deeply immersed in both the science and art of restorative care, I often encounter patients who are unsure whether to consult a general dentist or a restorative specialist. The overlap in services can be confusing, but there are fundamental distinctions that significantly impact patient outcomes, especially in complex cases. In this article, I will explore the key differences between general dentistry and restorative dentistry from a technical and clinical standpoint, drawing upon my experience at Dental Implant Partners in San Francisco.

What Is a General Dentist?
A general dentist serves as the cornerstone of a patient’s oral healthcare. This role encompasses a broad scope of preventive and diagnostic services, including routine exams, cleanings, fillings, and basic restorative treatments. General dentists are trained to manage a wide array of dental needs, often acting as the first point of contact for patients experiencing discomfort, oral infections, or functional issues. This makes them invaluable for early detection and long-term dental maintenance.
The educational foundation of a general dentist typically involves earning a DDS or DMD degree from an accredited dental school. This curriculum includes exposure to all dental disciplines, such as endodontics, prosthodontics, oral surgery, and pediatric dentistry, but the training remains generalized. While they may perform some complex procedures depending on their comfort level and continuing education, general dentists generally do not specialize in rehabilitative or full-mouth reconstructions. Their role is more akin to that of a primary care physician in medicine.
General dentists can provide crowns, bridges, partial dentures, and occasionally implants, but usually only for straightforward cases. Their treatment planning tends to be reactive and tooth-specific, rather than systemically integrative. For cases involving widespread tooth loss, collapsed occlusion, or severe wear patterns, the need for a higher level of interdisciplinary planning becomes apparent, which is where restorative dentists step in.
What Is Restorative Dentistry?
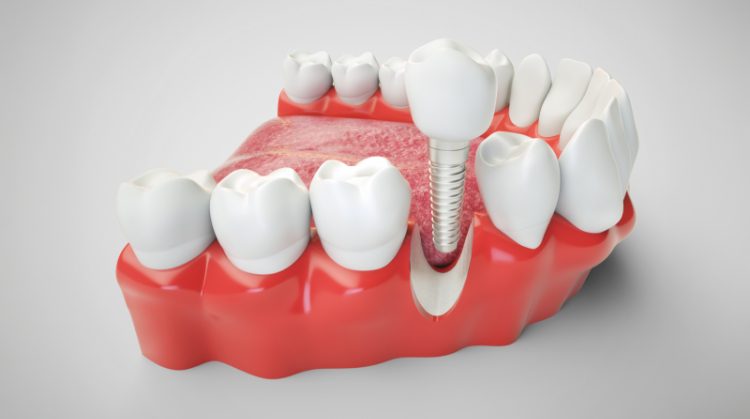
Restorative dentistry is focused on rebuilding and rehabilitating the oral structures for patients with complex dental conditions. This can involve replacing missing teeth with implant-supported prostheses, restoring the bite through full-mouth rehabilitation, and addressing collapsed vertical dimensions. In my practice, I specialize in comprehensive treatment plans that aim not only to restore esthetics but also to re-establish functional harmony across the dental arches.
This field requires extensive postdoctoral training and a high level of precision. Restorative dentists typically pursue advanced education in prosthodontics, implantology, occlusal analysis, and TMJ therapy. The learning curve is steep and continuous, as technologies and materials evolve rapidly. We rely heavily on diagnostic tools such as cone-beam CT scans, digital smile design software, and intraoral scanners to tailor restorations that integrate with the patient’s existing anatomy and function.
The scope of restorative dentistry also encompasses a deeper understanding of biomechanics, occlusal relationships, and how the temporomandibular joint interacts with dental prostheses. Our treatment is driven by system-wide evaluation rather than isolated issues. For instance, when planning a full-arch implant case, I assess everything from bone density to esthetic symmetry to long-term load distribution, ensuring that the result is stable, functional, and esthetically pleasing.
Education and Advanced Training
Both general and restorative dentists begin with a foundational dental degree, but restorative dentists typically extend their education through residencies, fellowships, or intensive continuing education. These programs dive into highly technical subjects such as advanced prosthodontics, occlusion theory, maxillofacial prosthetics, and digital workflows. This additional training allows restorative dentists to perform complex procedures with a greater level of accuracy and predictability.
While general dentists often pursue continuing education as well, their focus is generally broader and less specialized. They may take courses in cosmetic bonding or single-implant placement, but rarely engage in full-mouth rehabilitation training unless they are transitioning into a more specialized practice. The volume and complexity of cases handled in general practice also differ significantly from those in a restorative setting.
My own continuing education has involved advanced implantology programs, courses on full-arch reconstructions, and hands-on training in occlusal rehabilitation. These allow me to manage cases involving long-span bridges, bruxism-induced damage, and failing dentition with confidence. Staying updated with evolving materials and software tools is crucial, and the commitment to lifelong learning is a hallmark of any true restorative practitioner.
Diagnostic Techniques and Planning Approach
A major differentiator between general and restorative dentistry lies in the depth of diagnostic evaluation. General dentists usually work with standard periapical or bitewing radiographs, supplemented by clinical exams and patient history. These tools are effective for basic diagnosis and treatment planning, particularly for caries, mild periodontal disease, and simple restorations. They provide a snapshot but not the full systemic view needed for more involved procedures.
Restorative dentists rely on an expansive diagnostic toolkit that includes cone-beam CT imaging, full-arch digital scans, photographic documentation, and articulation-based occlusal analysis. These tools allow us to construct a complete digital or analog representation of the patient’s oral condition. We evaluate everything from bone contours and joint health to vertical dimension loss and esthetic line symmetry before initiating any treatment.
Planning a complex case involves staging and interdisciplinary coordination. I often work in collaboration with periodontists, oral surgeons, and lab technicians to execute each phase with precision. The planning process may also include diagnostic wax-ups, mock-ups, and provisional restorations to test function and esthetics before final prostheses are fabricated. This level of foresight and customization goes beyond the typical scope of general practice.

Treatment Complexity and Case Types
General dentists primarily manage routine care and moderate restorations. Their patients often present with isolated cavities, minor esthetic concerns, or single-unit crown needs. These cases are generally resolved within a few appointments and rarely involve surgical components or full-arch planning. For most patients, this level of care is sufficient to maintain oral health and function.
Restorative dentists, in contrast, deal with patients who have extensive needs, such as those with multiple missing teeth, worn dentitions, failed restorations, or complications from prior dental work. These cases often require surgical intervention, tissue regeneration, and prosthetic customization. Managing such complexity necessitates a deeper clinical skill set and advanced planning to avoid future complications.
In my daily practice, I see patients with severe occlusal collapse, advanced bone loss, and multi-implant rehabilitation needs. These cases are rarely completed in a single visit and may span several months. Each phase is meticulously executed to ensure stability, esthetic balance, and long-term functionality. This depth of care is the defining characteristic of restorative dentistry.
Materials and Prosthetics Used
General dentists often use conventional materials like composite resin, amalgam, and porcelain-fused-to-metal crowns for basic restorations. These materials are cost-effective and versatile for treating cavities, chipped teeth, or minor cosmetic issues. While many general dentists are proficient in cosmetic bonding or single-unit crowns, the complexity and customization are typically limited by material and procedural scope.
Restorative dentistry employs high-performance materials such as zirconia, lithium disilicate, hybrid ceramics, titanium implants, and custom abutments. These materials offer superior strength, esthetic translucency, and biocompatibility, making them ideal for long-span bridges, full-arch restorations, and implant-supported prostheses. Precision in fabrication is crucial, and many restorations are created using CAD/CAM technology and advanced laboratory techniques.
The difference is not only in the material but in how it is used. When I design a zirconia full-arch prosthesis, I take into account load distribution, opposing arch interaction, and gingival integration. Every contour is mapped for functional harmony. This level of design sophistication is not typical in general practice, where the focus is on broader treatment accessibility and efficiency.
Use of Technology and Digital Dentistry
Digital technology is rapidly reshaping both general and restorative practices, but its integration is more deeply embedded in restorative workflows. While many general dentists use intraoral scanners and digital X-rays, restorative dentists often go further by implementing 3D treatment planning, guided surgery systems, and digital occlusal mapping. These tools enable high-precision planning and predictable surgical outcomes.
In my restorative workflow, I employ cone-beam computed tomography (CBCT) to map bone anatomy, digital smile design for esthetic planning, and guided implant systems to ensure minimally invasive, accurate placement. These tools minimize chair time and surgical risks while improving long-term results. The use of digital articulation and mock-ups also allows patients to preview their final smile before treatment begins.
General dentists may incorporate some of these technologies but are less likely to invest in comprehensive systems due to costs, training demands, or the nature of their patient base. In restorative practices, however, digital integration is not optional; it is essential. It enables higher-quality outcomes, particularly in full-mouth cases and precision implant prosthodontics.
Time and Cost Considerations for Patients
The time and financial investment required for restorative dentistry is significantly higher than that for general dental procedures. Complex cases often span several appointments over many months, involving surgical phases, healing time, and prosthetic fabrication. The materials used, technology involved, and specialist coordination also contribute to the higher cost structure.
General dentistry services are usually less time-consuming and more affordable, especially for patients with insurance. Preventive care, fillings, and simple crowns are often covered by dental plans, making them more accessible. While general dentists may offer some elective cosmetic services, these are typically limited in scope and cost compared to full-mouth rehabilitation or multi-implant solutions.
Restorative patients often require customized financial planning, including phased treatment options, financing solutions, and insurance coordination. In my practice, we discuss the long-term value of care, how properly restored function and esthetics can prevent further deterioration and reduce future costs. It’s an investment not just in oral health, but in quality of life.
Collaborative Care Between Providers
Effective dental care often involves collaboration between general dentists and specialists. In fact, many of my restorative cases are referred by general dentists who recognize the need for advanced intervention. We work together to ensure the patient receives continuity of care, from preventive maintenance to final prosthetic delivery.
Collaboration requires clear communication, shared diagnostics, and mutual respect for each provider’s expertise. I provide referring dentists with detailed treatment plans, progress updates, and post-restoration maintenance guidelines. Once the complex phase is completed, patients often return to their general dentists for routine follow-up, cleanings, and monitoring.
This team-based model ensures the best outcome for the patient. General dentists focus on early detection and maintenance, while restorative specialists like myself address complex rehabilitative needs. Each plays a vital role in the broader spectrum of oral health, and together we create a seamless patient journey from prevention to transformation.
When to See a Restorative Dentist
Patients experiencing significant tooth loss, extensive wear, multiple failing restorations, or TMJ issues may benefit from seeing a restorative dentist. These conditions often require multidisciplinary treatment planning and prosthetic reconstruction, which goes beyond the scope of general practice. If you’ve been told your case is too complex for a standard solution, a restorative consultation is advisable.
Other indicators include collapsed bite, difficulty chewing, esthetic dissatisfaction despite multiple prior treatments, and implant failure. In these cases, surface-level fixes do not address the underlying issues. A restorative dentist conducts a holistic analysis and develops a strategic, phased plan that addresses function, structure, and appearance comprehensively.
At Dental Implant Partners, I take the time to educate patients on every aspect of their condition and treatment options. The goal is not just to fix teeth, but to rebuild a healthy, functional, and beautiful smile that lasts. If you suspect your dental needs go beyond routine care, it may be time to explore the benefits of restorative dentistry.

Restore Your Smile with Dental Implant Partners
At Dental Implant Partners, restorative care is not just our specialty, it’s our passion. For over 25 years, I’ve had the privilege of leading this prosthetic-focused practice in the heart of San Francisco. What began as a solo practice has grown into a team of dedicated professionals, including highly trained prosthodontists, general dentists, and hygienists who are not only exceptionally skilled but also deeply committed to patient care. Our hygienists, many of whom were trained as dentists themselves, have been with us for years and are beloved by our patients for their warmth and precision.
We offer a full spectrum of restorative treatments, ranging from simple fillings and esthetic veneers to full-mouth rehabilitations supported by dental implants. Our expertise extends to designing and delivering beautifully crafted dentures for patients for whom implants may not be the right choice. Every treatment plan is approached with individualized care, scientific rigor, and a focus on long-term outcomes. Whether you need a single crown or a complete smile reconstruction, our team takes the time to do it right, using the best materials and latest techniques in a serene, beautifully designed suite overlooking the San Francisco Bay.
If you are considering restorative dental care or are unsure whether your case requires a general or restorative approach, we invite you to reach out to us. Let’s talk about your goals and develop a thoughtful, customized plan to restore your smile. We love our work, and we would love to help you take the next step toward dental health and confidence. Contact us today to schedule a consultation and experience the difference at Dental Implant Partners.